5 Promising Developments in Childhood Epilepsy
Children with epilepsy sometimes endure dozens to hundreds of seizures in one day. If you’ve never witnessed a seizure, it can take a variety of forms, such as a child staring off into space, jerking movements in the arms or legs, stiff body, breathing issues, loss of bowel or bladder control, appearing confused, or even losing consciousness. For the 456,000 children under the age of 17 who have been diagnosed with epilepsy nationwide, this can be their reality.
Epilepsy is a neurological disorder that sometimes fades as children age, but other times it can be something they struggle with for decades or for life. In adults, epilepsy is divided into four main classifications: Focal, Unknown (whether focal or generalized), Generalized and Unclassified, with each of the seizure classes having specific descriptors. In young children and infants, classification can be slightly different, with a stronger emphasis on the use of electroencephalography (EEG) to aid in diagnosis.
Most children with epilepsy see relief after trying one or two medications, said Ravindra Arya, MD, DM, pediatric epileptologist at Cincinnati Children’s Hospital and Medical Center. But, around 30% of childhood epilepsy cases are considered “drug resistant,” meaning traditional medication options haven’t helped.
But advances in treatment options for pediatric epilepsy offer a brighter future for kids in which medicine hasn’t worked. From developing improved diagnostic processes to less-invasive procedures, researchers are hard at work imagining a future where all kids with epilepsy have effective treatment plans.
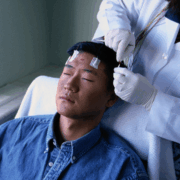
Not all children with epilepsy will need surgery, but imagine this for a child who needs it: They have just endured a surgery to insert implants into their brain, all for the purpose of mapping the source of seizures. Just days after, with anesthesia barely out of their systems, they have to undergo tough testing, answering questions, reading flashcards, and engaging in other language and communication tasks for hours. Yet, brain mapping is necessary to minimize the risk of lost brain function during surgery.
“They have electrodes in their brain. They are tied to the EEG machine. They are in an unfamiliar hospital environment, and you are asking them to do these artificial tasks repetitively for hours. That’s the current standard of care,” Dr. Arya said.
And that doesn’t include the difficulties some kids may have with testing in general, such as behavioral or communication challenges.
These facts were the motivation behind a new testing process available for some children called Behavior-iEEG-Spectral-Power Correlation (BESPoC). Dr. Arya was the corresponding author on the study, published in the Annals of Neurology in August 2025.
Dr. Arya explained that the new process is much faster and easier and involves a simple and short conversation with a family member, rather than hours of arduous tasks. Turns out, the “naturalistic conversation” actually leads to better outcomes, and it can happen in just five minutes.
While the process still involves those electrodes on the brain in a surgery format, Dr. Arya hopes to expand to non-invasive sensors in the future and to study how the brain works during natural behaviors—like video gaming—during the diagnostic process.
Recent gene therapy advancements include work by Capsida Biotherapeutics and scientists to better understand STXBP1, a mutation often associated with epilepsy. A recent review found that vector gene therapies have grown significantly in the past decade, which is encouraging for all epilepsy treatments.
“Gene therapy is emerging as one of the most promising treatments for childhood epilepsy, offering targeted interventions based on the underlying genetic cause,” said Nicole H. Cobo, MD, pediatric neurologist at Miller Children’s & Women’s Hospital Long Beach and MemorialCare Long Beach Medical Center in California. “This approach enables precision medicine, tailoring treatment to the unique genetic profile of each child. Genetic testing is becoming increasingly critical for the appropriate treatment and prognostication in pediatric epilepsy.”
3. Improvements in Deep Brain Stimulation
Deep brain stimulation (DBS) has been around since the 1990s, originally used for essential tremors and Parkinson’s disease, explained Chris Conner, MD, PhD, director of functional neurosurgery at the University of Connecticut Health in Farmington. More recently, some “intrepid neurosurgeons and neurologists” started using it with epilepsy patients too, he said.
Epilepsy is a single word that covers many different issues. “There are some patients where we can take out the part of the brain that starts the seizure. There are some where we cannot narrow it down and remove something—those patients are the ones to whom we offer electrical stimulation,” Dr. Conner said.
Some manufacturers, such as Medtronic, have newer technology that can apply electricity to the brain, but also record it, a process Dr. Conner described as similar to a thermostat. “It senses what is going on and then adjusts how the electricity is delivered. I think that the technology is still in its infancy, but we’re getting there,” he said. “This ‘brain sensing’ will help improve how effective DBS is at treating epilepsy and make it easier for physicians to program the system.”
New types of approaches that greatly reduce the risks of surgery to treat epilepsy are becoming more widely available, including one nicknamed LiTT — which stands for laser interstitial thermal therapy, which is short for magnetic resonance-guided laser interstitial thermal therapy (MRgLITT) for epilepsy.
A 2025 pooled pediatric analysis combined results from 354 children who had the LiTT procedure. After about 16 months of follow-up, 57% of the kids had no disabling seizures. The success rate was even higher in children with a type of lesion called hypothalamic hematoma, which is a benign brain growth that often triggers severe seizures.
One of the study’s researchers was Ian S. Mutchnick, MD, a pediatric neurosurgeon at Norton Children’s in Louisville, Kentucky. “LiTT allows for the destruction of lesions—cancer, epilepsy and even some vascular—with minimal damage to the overlying tissue,” Dr. Mutchnick said. “This is incredibly useful when treating deeper lesions. Where traditional open approaches have sought to only reduce the amount of unavoidable damage required to get to the lesion, LiTT allows us to treat lesions with only minimal amounts of collateral damage.”
Dr. Mutchnick called the procedure “very promising” and said they are currently studying how to best apply the methodology, or how to determine who should get the procedure. He estimated LiTT could help around 20% to 30% of kids with epilepsy.
5. A ‘Pacemaker’ for the Brain
It may sound too good to be true for kids suffering numerous seizures for a long time: a device implanted in the brain that stops seizures before the individual even senses they are starting.
Yet, that is becoming reality for some of the hardest cases to treat, through a pacemaker-like procedure called responsive neurostimulation (RNS). Though RNS is not new—it was developed around a decade ago—doctors are now beginning to use RNS in children, not just adults.
In February 2025, Virendra R. Desai, MD, surgical director of the Comprehensive Epilepsy Center at Children’s Hospital Los Angeles, performed the first procedure on a child with epilepsy in a five-hour surgery. He shared in a hospital blog: “It works really well. People across the world have reported an average seizure reduction of about 80%. There is a range of responses, but many patients see a greater than 90% reduction in seizures.”
Dr. Desai emphasized this technology helps those who have already tried without success vagal nerve stimulation, diet changes and other procedures.
Looking at the progress and new and promising treatments for childhood epilepsy, Dr. Mutchnick echoed a sentiment felt from other physicians treating this condition: “I’m very excited about what lies ahead. … By taking a more quantitative approach we can greatly improve both diagnosis and treatment.”