Your Eyes Could Be Early Warning Signs for These 6 Diseases
You’ve probably heard the old expression “the eyes are a window to the soul.” In fact, in many ways, the eyes are an extension of the brain. The retina and optic nerve are part of the central nervous system, meaning changes in the brain can sometimes be detected through the eyes.
It’s important to take vision changes seriously—and not only to protect your eyes. Changes may simply be signs you’re getting older, but they can also suggest the presence of other kinds of disease.
Here are a few ways your eyes can give you and your doctors insight into what’s happening in your brain:
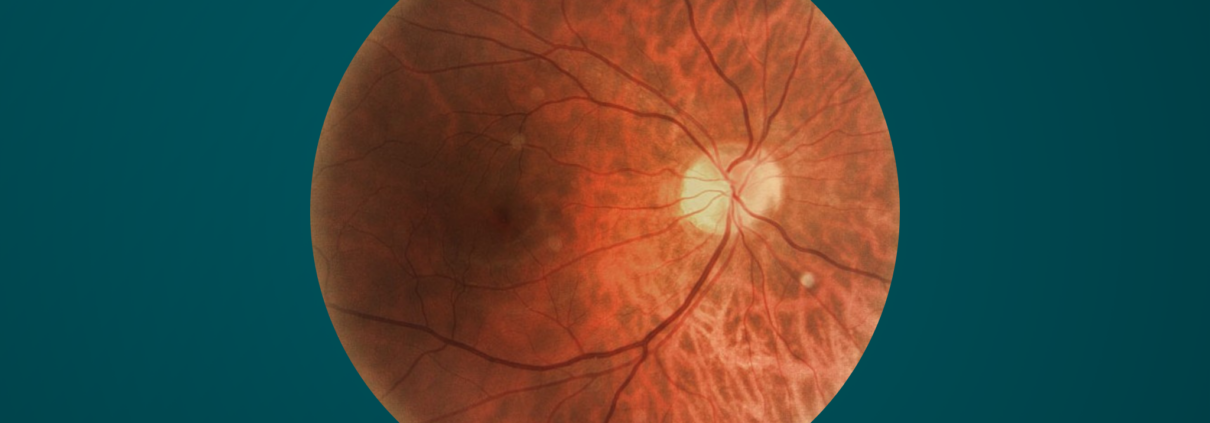
1. Alzheimer’s disease. The retina is a layer of specialized cells at the back of your eye that captures light and converts it into electrical signals that the brain interprets as images. The retina could reveal evidence of Alzheimer’s disease, a progressive form of dementia that’s also the most common form of dementia. According to research, eye doctors may be able to get a glimpse in the retina of the presence of beta-amyloid plaques—the sticky protein fragments that are the main hallmark of Alzheimer’s disease. These findings are still being studied and are not yet part of routine clinical screening, but they highlight the growing interest in the eye as a potential biomarker for neurodegenerative disease.
2. Multiple sclerosis. Vision problems are one of the first noticeable signs of multiple sclerosis (MS), according to the National Multiple Sclerosis Society. The most common symptoms of this autoimmune neurological disorder are:
- Diplopia, which is double vision
- Nystagmus, which is rapid, involuntary eye movements
- Optic neuritis, which is pain or vision loss caused by inflammation to the optic nerve.
In MS, the immune system attacks the protective myelin coating around nerve fibers. When this inflammation affects the optic nerve, it can disrupt the transmission of visual signals from the eye to the brain.
In fact, people who are experiencing pain or inflammation in their optic nerve should get some additional tests because research suggests that optic neuritis can be one of the first signs of MS. About half of people with MS experience optic neuritis at some point.
3. Brain tumors. What if you knew that vision changes should prompt you to seek evaluation for a possible brain tumor? That makes annual doctors’ appointments seem even more critical, right? In fact, blurry vision, a dead spot in your field of vision, and double vision can all be signs that a mass or tumor is pressing on the optic nerve, which carries signals between your eyes and your brain. Other signs that could possibly signal the presence of a tumor include a decrease in visual acuity (being able to see clearly and correctly) and loss of peripheral vision (your side vision).
4. Intracranial hypertension. With advancements in optic nerve imaging came the ability to detect possible signs of intracranial hypertension. This condition is different from systemic high blood pressure or “hypertension,” although both can affect the visual system in different ways. Intracranial hypertension—or increased pressure inside the head—can create swelling in the optic disc, which is the head of the optic nerve where it connects with the back of the eye. This causes a serious condition called papilledema, which is a medical emergency that needs to be treated so you don’t lose your sight. If you ever experience double vision or short episodes where your vision goes blurry or blacks out and then comes back, it could be a sign of papilledema. Seek medical attention immediately.
5. Stroke. When your eye doctor dilates your eyes and performs a comprehensive eye examination, they can see the tiny blood vessels in your eyes. This can allow them to spot blood clots that can block arteries supplying blood to your retina, a condition known as retinal artery occlusion, or an “eye stroke.” Your eye doctor may also notice signs that you’re at elevated risk for having a stroke, like blood clots or plaque deposits in the arteries that could break off and travel to the brain.
6. Vascular disease. A dilated eye exam can also reveal any visible bleeding that could signify the development of vascular disease, such as the presence of subconjunctival hemorrhages, which are small red patches where a blood vessel has burst in the white part of the eye. With older adults, these can be a sign of systemic vascular disease (which can, in turn, increase the risk of having a stroke.)
Here’s one more fascinating way your brain and your eyes are connected:
Brain plasticity. Years ago, scientists thought that the brain was essentially fixed, unchangeable, especially after a certain age. Now we know that’s not true—and the brain may be even more plastic and malleable than previously thought.
Recently, research from MIT found that older children with congenital cataracts who underwent cataract removal surgery were able to gain the ability to recognize faces, detect motion, and perform other visual tasks after their sight was restored. Their brains were able to respond to a major change and adapt, a phenomenon known as neuroplasticity. This suggests that even after periods of limited visual input, neural circuits responsible for perception can reorganize and regain function.
The brain does indeed adapt to changes, like when you suffer an injury. For example, when someone loses their vision, their brain may undergo a process of reorganization that allows them to more effectively process incoming information by using their other senses. That doesn’t mean there aren’t limits to neuroplasticity. However, research does suggest that the brain adapts and changes throughout a person’s lifespan.
The close relationship between the eyes and the brain means that vision changes are never just about eyesight: They can offer important clues about overall neurological health.