How different strokes impact different brain functions
Strokes can happen anywhere in the brain and the symptoms can vary dramatically based on exactly which part of your brain is affected.
There are two main types of strokes, explained Dr. Alyse Sicklick, MD, a physical medicine and rehabilitation specialist at Gaylord Specialty Healthcare in Connecticut. The two types are ischemic (pronounced iz-kee-mik) and hemorrhagic.
In an ischemic stroke, a blood clot blocks blood flow to a portion of your brain, and the cells there are starved for oxygen. Some ischemic strokes are transient, meaning the symptoms only last a few minutes, but others can cause permanent damage to the brain. In a hemorrhagic stroke, a blood vessel in your brain bursts, causing bleeding in your brain.
Both types of strokes end up killing brain cells. Scientists estimate 1.2 million brain cells die every minute a region of the brain is deprived of the oxygen in blood. As more and more brain cells die, stroke symptoms get worse, according to Dr. Anmar Razak, associate professor of neurology and chief of cerebrovascular neurology and neurointervention at Michigan State University. Because each part of your brain has its own specialized functions, the location of the stroke determines exactly which symptoms you might experience as a result of those cells dying.
“If you think about the brain blood supply, it’s almost like a branching tree. Blood vessels start as main stems or main blood vessels from the heart and then they branch out into the neck, and as they go up into the head, they continue to branch out into smaller and smaller branches,” Dr. Razak said. “Each of these blood vessels supply a particular area in the brain. Depending on where that blockage is, you will have different types of symptoms.”
Strokes in the Frontal Lobe
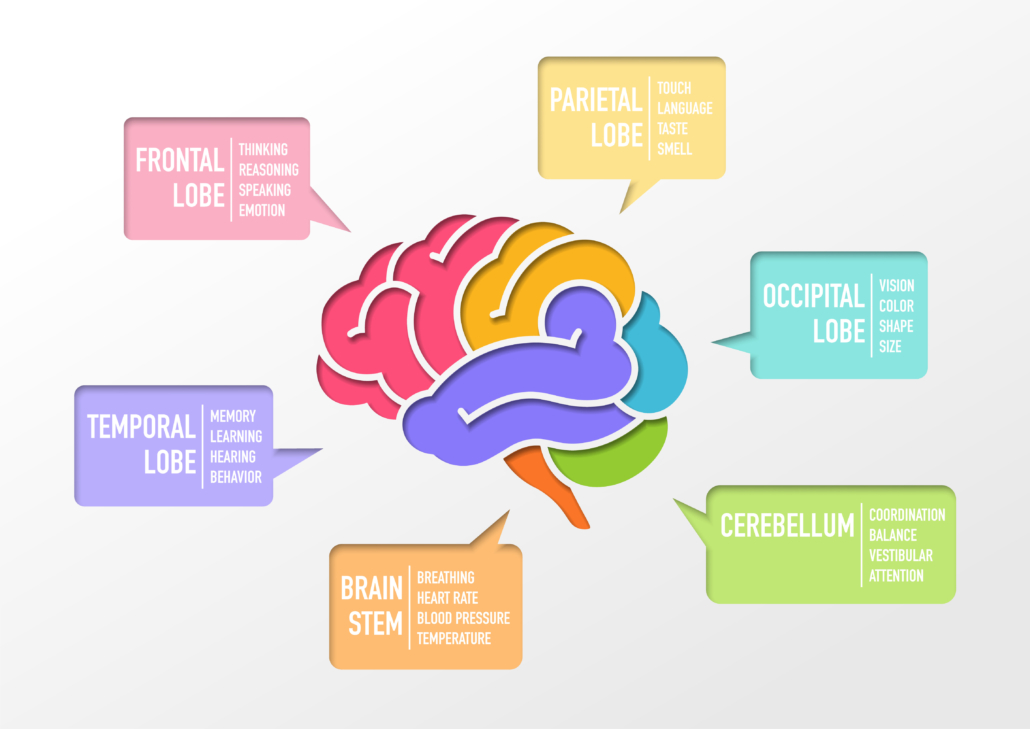
Your brain is made up of four lobes: the frontal lobe which sits right behind your forehead, the parietal and temporal lobes which are in the middle between your ears, and the occipital lobe at the back of your brain. Behind the occipital lobe and a little lower down, near the base of your neck is the cerebellum, a smaller region that almost looks like a mini brain.
Most people having strokes have weakness in their face or one arm. If you ask them to smile, one side of their mouth might move more than the other. Their speech may be irregular. If you ask them to lift their arms, they may not be able to raise one as high as the other. These symptoms are typically caused by damage to the motor cortex, which is situated in the frontal lobe.
Dr. Razak explained that there is a large amount of space in our brains dedicated to the movement of our arms and face. “So statistically speaking, if there is a blockage somewhere it is likely that it will impair, to some degree, the ability to move the face the ability to move the arm.”
Still, researchers found in 2017 that 14.1 percent of patients who were having strokes did not show any these common symptoms: Instead, many of them instead showed symptoms of stroke in other parts of the brain. Then, of course, there are prefrontal strokes. Patients who have that flavor of strokes sometimes will experience prominent leg weakness and personality or behavior change instead of arm pain or speech change.
The Temporal and Parietal Lobes
The temporal lobe is home to the brain’s language centers. If a stroke damages a region in the temporal lobe called Wernicke’s area, a patient may suddenly struggle to understand speech and written language. Wernicke’s aphasia in its purest form is fluent speech that has no meaning whatsoever—a “word salad” of nonsensical speech. If a stroke damages a part of the posterior frontal lobe called Broca’s area, a patient may still understand speech adequately, but not be able to speak in meaningful sentences.
The parietal lobes help manage and integrate multiple sensory processes in the brain, including the senses of touch, pain, temperature, and joint position. They are also responsible for integrating our senses of vision and hearing together as well. This integration helps us understand how our body is feeling and operating in relationship to the world around us.
A stroke in the right side of the parietal lobe can cause a unique symptom called left-sided spatial neglect. In this case, a patient’s vision is fine, but the patient will start to ignore the left side of their visual field. For example, a patient may not realize that they have only eaten food off the right side of a plate. The presentation is dramatic. Right-sided neglect is actually fairly rare and difficult to detect—this is because the right spatial field is redundantly processed by both the left and right hemispheres.
Dr. Tanu Garg, MD, a vascular neurologist at Houston Methodist Hospital emphasized that such strokes can affect more than just spatial awareness: These strokes can also change a person’s awareness of his or her own body.
“The reason why that’s important is because when you have a stroke on the right side of your brain, it causes weakness on the left side, but it also causes the person to feel like that they their left side is not there or they don’t have a left side,” she said.
Strokes in the Occipital Lobe and Cerebellum
Strokes that hit the optic nerve or the occipital lobe can cause visual disturbances such as blind spots or double vision. People also experience conditions that seem almost paradoxical. For example, some people have blindsight, a condition in which a person will say that they cannot see, but will behave as though their vision is still intact. They’ll avoid obstacles while walking but say they cannot see those obstacles. Strokes can also cause the opposite effect, cortical blindness, a condition in which people are blind, but think they can still see.
These disturbances could also worsen your balance and make it difficult to walk.
One of the cerebellum’s main jobs is to help you control movement and balance. If a stroke happens in this brain region, Dr. Garg said, patients might not experience any of the more common stroke symptoms. Instead, they may “feel dizzy or like they cannot walk properly,” she said, adding, “these strokes are very, very important because not being able to walk and being dizzy all the time is very disabling.”
That isn’t the only reason why these strokes are important; cerebellar strokes also tend to swell and kill young people.
Rehabilitation
Strokes can be devastating. and even fatal. At the same time, many people not only survive, but manage to regain most or all their function back. In one large study, 75.4% of stroke patients survived. In the same study, three to six months of intensive rehabilitation, including physical and occupational therapy, improved patients’ independence and quality of life after a stroke.
Rehabilitation after stroke usually comprises a few days of inpatient care, followed by weeks to months of outpatient care. The care team can include nurses, physical therapists, speech therapists, and more. A neuropsychologist, a psychologist with a doctorate who specializes in the connection between the brain and behavior, can help design and implement rehabilitation. The techniques used by a rehab team will vary depending on a patient’s symptoms. If a patient has symptoms of neglect, their rehab specialist may stand on their left side while speaking to them in an attempt to encourage the patient to look toward that neglected side. Dr. Garg said a specialist also might put weight in a patient’s left hand so the patient feels sensation through the whole neglected arm.
To help with vision loss, occupational therapists can help train stroke survivors to differentiate between light and darkness and identify movement. Researchers are also evaluating a variety of experimental techniques such as transcranial brain stimulation.
Dead brain cells won’t grow back after a stroke, but throughout a patient’s rehabilitation, neighboring cells can learn new functions and take over for those cells that died, explained Dr. Razak.
Dr. Sicklick added that this plasticity means that, “some people can improve even years after a stroke if given the right intervention.”
This article has been factchecked. For more about that process, click here.